About 2.2 million people in Australia are suffering from osteoarthritis, according to the Australian Bureau of Statistics' 2017-18 data. Most of whom are women aged 75 years and over, but the condition usually starts developing from age 45 onwards. Osteoarthritis is the most common type of arthritis that develops gradually with age. This article takes you through its causes, symptoms and possible treatment methods.
What is Osteoarthritis?
Osteoarthritis (OA) is a degenerative condition that mainly affects joints in the hands, hips, knees, spine and ankles. It occurs when the ends of bones located in the joints are damaged due to the disintegration of the cartilage, the soft tissue that covers the ends of bones. The loss of cartilage leaves the bones rubbing together, which causes joint pain, swelling, tenderness and limited range of motion.
Normal joints have all their essential components, namely bone, joint capsule, synovial tissue and fluid, cartilage, tendons and ligaments, neatly arranged in place to prevent friction and damage. People with osteoarthritis have lost most of these components, so they experience pain as their bodies cannot hold up high amounts of stress on joints. Performing normal activities like walking, cooking or even getting dressed becomes an ordeal for them, hence affecting the quality of their life. If left untreated, this condition can lead to permanent disability.
Common Symptoms of Osteoarthritis
The development of osteoarthritis takes years, with pain usually starting at one joint or with finger joints. However, the symptoms tend to get worse over time. As OA causes more symptoms, the joint may become less flexible and eventually may not be able to fully bend. When joints are moved, the irregular surfaces cause them to grind, causing excruciating pain, especially in the weight-bearing joints such as the ankles, knees and hips. Apart from pain, people with osteoarthritis also manifest the following symptoms:

- Joint stiffness
- Joint instability
- Bony growth and enlargements
- Decreased range of movement
- Popping sound from the used joint
- Inflammatory conditions
Causes and Risk Factors of Osteoarthritis
Joint injury or daily activities that require repetitive movements which strain one joint, or group of joints, can cause damage to the cartilage. Excess weight also causes more stress on joints, particularly in weight-bearing areas. In fact, obese individuals have an increased risk of developing OA and other related musculoskeletal conditions. Other factors that may increase the risk of osteoarthritis include:
- Age - the older a person is, the higher their chances of developing the condition
- Genetics - a family history of osteoarthritis makes one more susceptible to the joint disease
- Medical condition - secondary osteoarthritis usually develops in people whose cartilage has been damaged by another health condition. People with hand OA are also more likely to develop knee osteoarthritis.
- Joint disorders - a congenital joint contracture puts one at risk of osteoarthritis
Diagnosis of Osteoarthritis
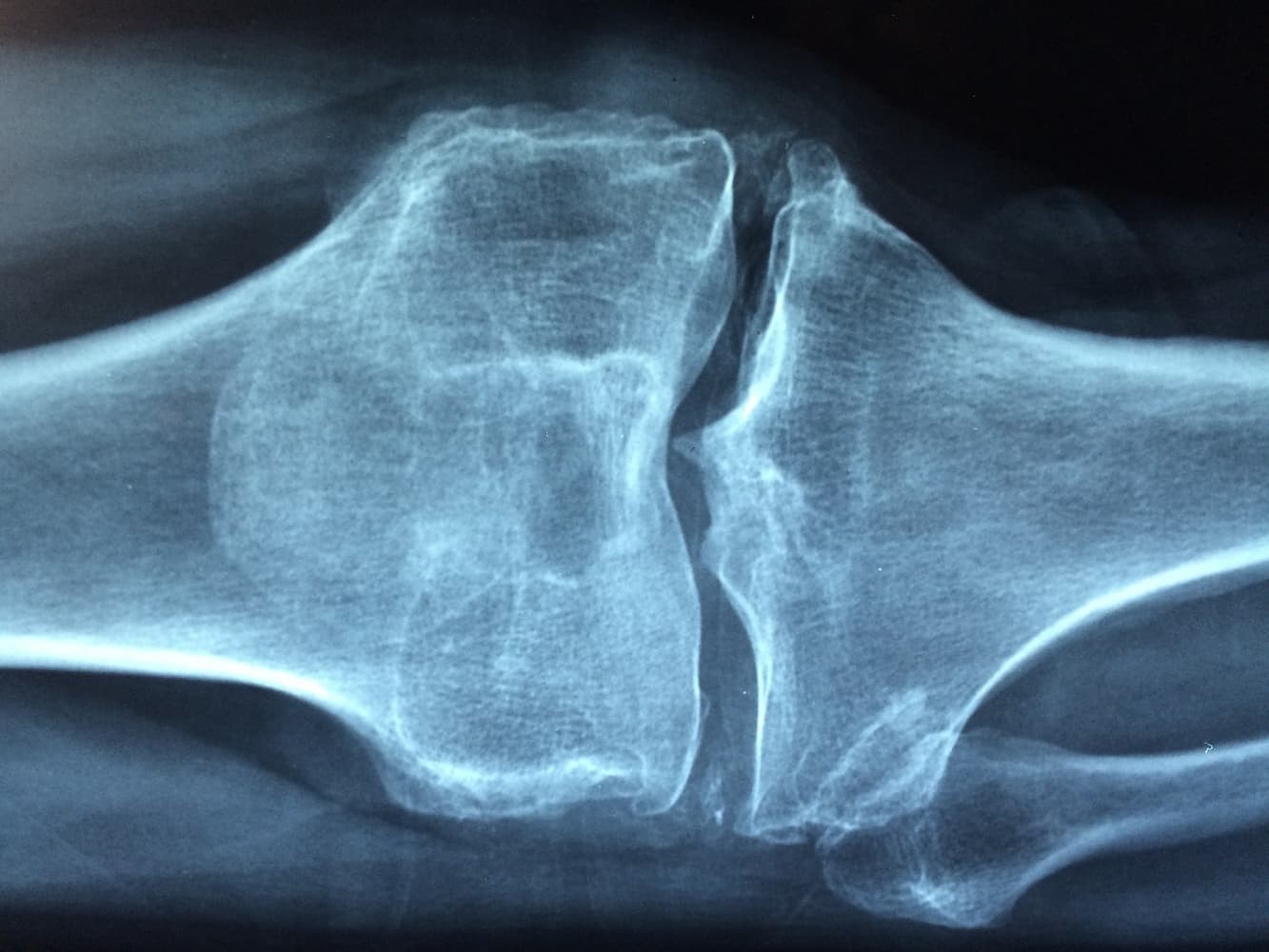
A medical health professional, who specialises in bone and joint diseases, will conduct a thorough physical examination and a couple of tests on the patient to diagnose OA. Taking X-rays helps them see whether or not the patient has a healthy cartilage intact as the distance between the bones will give the answer away.
Doctors can also use magnetic resonance imaging (MRI), another imaging technique that uses strong magnetic fields to capture images of the structures and activities of bones and joints.
Arthrocentesis is an invasive diagnostic procedure that involves drawing a small amount of joint fluids from the affected joint using a sterile needle. The fluids are then analysed in the laboratory to find out if the pain is caused by gout, rheumatoid arthritis or an infection rather than OA.
Treatment for Osteoarthritis
Osteoarthritis is irreversible. Once symptoms of the condition start to manifest, you can only control them with the appropriate treatment methods to prevent them from getting worse. Most doctors would prescribe nonsteroidal anti-inflammatory drugs to relieve the pain. They would also use hyaluronic acid injections on patients with severe symptoms to lubricate the affected joint and make it less painful.
An occupational therapist can also educate patients on how to move their bodies properly to avoid putting so much stress on their joints. They may also recommend assistive devices to increase the patient's comfort and allow them perform their everyday activities with less pain.
Some forms of complementary therapies can also help with the management of osteoarthritis. Physical therapy is one of them. In fact, it's in demand among patients with OA and other types of arthritis thanks to its efficacy in reducing pain, improving flexibility and increasing range of motion.

Diet, lifestyle and maintaining a healthy weight are pivotal to the improvement or progression of osteoarthritis symptoms. Combining the appropriate medication with regular exercise, nutritious meals and ample sleep will significantly reduce joint pain and swelling. Certain home remedies like the application of cold therapies on sore joints can also improve symptoms without posing any side effects. If you wish to explore more natural treatments for osteoarthritis, check out the Natural Therapy Pages' comprehensive listing of natural health practitioners to find a qualified practitioner in your area whom you can work with.
|
Do you have a natural health & wellness business? |









